Repaglinide is an active ingredient that is used in type 2 diabetes mellitus when dietary measures, weight reduction and physical training do not sufficiently lower blood sugar. By inhibiting the potassium channels of the beta cells in the pancreas, the agent leads to the release of insulin. If the dosage and the conditions of use are adhered to, repaglinide is well tolerated.
What is repaglinide?
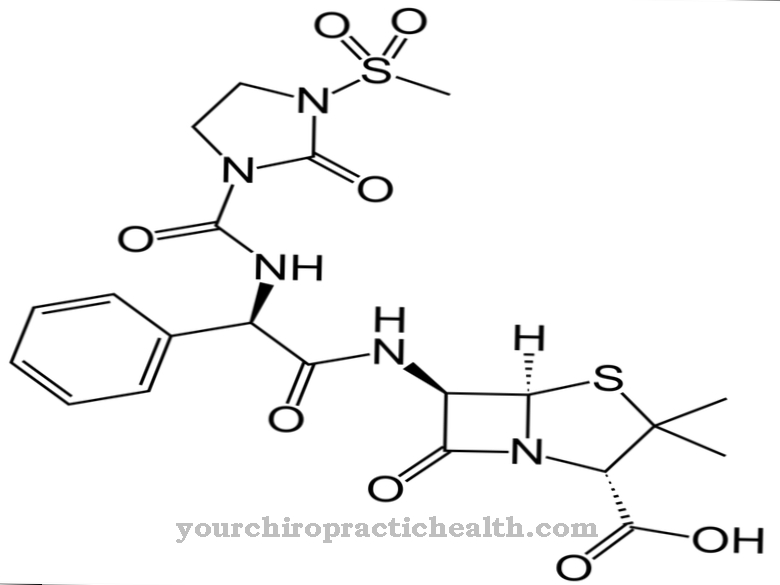
The oral anti-diabetic drug repaglinide increases insulin secretion from the endocrine pancreas. It binds specifically to potassium channels and thus causes insulin to be released.
Repaglinide belongs to the glinide group of active ingredients and is a benzoic acid derivative. It only works in the presence of glucose and has a short duration of action.
Pharmacological effect on the body and organs
The drug repaglinide is rapidly absorbed from the gastrointestinal tract after oral intake. The maximum plasma concentration is reached after one hour and quickly falls again. After 4-6 hours, the drug is completely eliminated.
The pharmacological effect of repaglinide consists in the inhibition of the ATP-dependent potassium channel of the beta cells of the pancreas. The potassium channel is a large complex of different binding sites for the body's own molecules. Adjacent membrane proteins, the sulfonylurea receptors, regulate the opening of the channel. Endogenous molecules, but also drugs such as repaglinide, interact with these specific receptors. The higher the affinity for the receptors, the more potent the drug is. The inhibition of the potassium channel leads to a depolarization of the beta cells with subsequent opening of the calcium channels. The increased calcium influx into the beta cells then induces the release of insulin.
Repaglinide works quickly and only against postprandial blood sugar. In particular, the effective lowering of postprandial blood sugar is currently considered to be important in reducing long-term cardiovascular events. In addition, there are fewer hypoglycemias because on the one hand the duration of action is short and on the other hand glinides only inhibit the potassium channel in the presence of sugar. As a result, the effect of repaglinide is weakened with falling blood sugar and the basal insulin secretion is not influenced.
The drug is mainly broken down by the hepatic system via the cytochrome P-450 enzymes CYP2C8 and CYP3A4. CYP28C plays a more important role here. Thus, the metabolism of the drug can be sensitively changed if the two enzymes are either inhibited or increased by other drugs. In particular, inhibition of the enzymes can lead to increased levels of repaglinide in the blood, which can potentially cause hypoglycaemia. 90% of the drug is excreted in the bile and only around 8% through the kidneys.
Medical application & use for treatment & prevention
Repaglinide is used in type 2 diabetes mellitus when normalization of blood sugar cannot be achieved through diet, physical training and weight reduction. It can be given as monotherapy, but it can also be combined with certain other antidiabetic drugs. Due to the rapid action of repaglinide, it is recommended to take it before main meals, ideally 15 minutes preprandially.
The starting dose is 0.5 mg and can be increased to a maximum single dose of 4 mg at intervals of 1-2 weeks if necessary. When switching from another antidiabetic drug to repaglinide, the starting dose is 1 mg. The maximum dose per day is 16 mg. The drug can also be used in cases of renal insufficiency, as repaglinide is hardly eliminated renally. However, depending on the case constellation, a dose reduction should be considered.
The blood sugar level and glycated hemoglobin (HbA1c) should be checked by a doctor on a regular basis to ensure adequate therapy. In addition, the effect of repaglinide may decrease over the course of treatment. This so-called secondary failure can arise due to the progression of diabetes mellitus or a reduced response to the drug.
Risks & side effects
There are some contraindications to the use of repaglinide. So it must not be used with a type 1 diabetic. Use is also contraindicated in the case of liver dysfunction or a derailment of glucose metabolism, in the sense of ketoacidosis. Likewise, the use in persons under 18 years of age and in adults over 75 years of age has not been adequately studied, which is why the administration of repaglinide is not recommended in these patient groups.
Repaglinide should not be used during pregnancy or breastfeeding. The risk of overdose, with subsequent hypoglycaemia, is low if the dosage is adhered to and sufficient meals are taken. In principle, however, hypoglycaemia is possible with repaglinide, as with other antidiabetic drugs. However, the short half-life of repaglinide reduces the risk. If hypoglycemic reactions occur, they are usually mild.
In very rare cases, further side effects are allergic reactions, liver dysfunction and eye dysfunction. Digestive tract complaints such as diarrhea or abdominal pain are more common.
There are a number of drugs that interact with repaglinide such that repaglinide's hypoglycemic potential is increased. These include in particular gemfibrozil, clarithromycin, itraconazole, ketoconazole, trimethoprim, ciclosporin, clopidogrel, other antidiabetic agents, monoamine oxidase inhibitors, ACE inhibitors, salicylates, NSAIDs, alcohol and anabolic steroids. In particular, a combination with gemfibrozil is not advisable because clinical studies have shown this drug to significantly increase the half-life of repaglinide and its potency. Hypoglycaemia could thus be triggered more frequently. On the other hand, there are drugs, such as rifampicin, that reduce the effect of repaglinide and thus make it necessary to increase the dose.
Other physical stress, such as infection, trauma, and fever, can also increase blood sugar levels, which may make it necessary to adjust the dose.